"LASERS vs SUPER luminescent LIGHT emitting DIODES" - A question of choice!
Although the basic principle of laser devices was developed at the turn of the century, rapid development in laser technology did not occur until the 1960's. In 1961, work began to assess the potential surgical applications of lasers, with the first successful surgical use being in the field of ophthalmology. The CO2 laser developed to overcome the early problems of high power machines became popular in the early 1970's, remaining the prime system in neurosurgery, dermatology and plastic surgery. Research into the development of and use of low energy lasers was begun almost a decade later by Professor Endre Mester in Budapest and simultaneously by Dr. Friedrich Plog in Canada. Since then, extensive research has been carried out in Russia and Eastern Europe, leading to the acceptance and clinical use of low intensity laser therapy. Later in the 1980's, reports began to be produced in Western Europe on the clinical use of low power lasers. Many of these reports tend to based on semi-conductor lasers and superluminous diodes.
Debate has arisen among many therapists regarding the use of semi-conductor lasers and superluminous diodes, referred to hereafter as SLD's, rather than true lasers. We need to answer a number of questions. Do they have different properties? Do they have different biological effects? Are there different safety parameters? Can they be used to treat the same conditions?
Looking first at some basic properties, both true lasers and SLD's produce monochromatic light, however, the true laser beam is also collimated. This means that it produces beams that are close to parallel. The small spot size produced by the beam is still maintained if the head is held away from the treatment area. The beams from SLD's have a greater level of divergence. In terms of beam size, the true laser has a smaller spot size of around 3mm² and SLD's are in the region of 20mm² . Whilst it would seem from these figures that the true laser has the advantage, its higher collimation means that the risk of eye damage is significantly greater with a true laser if the beam is accidentally viewed during treatment.
It is a common belief that the more powerful a piece of equipment, the better it is. At face value, the true laser has more power (between 30 and 200mW) than the SLD (power approx. 10mW). Higher average powers are believed to be best for musculoskeletal problems, lower powers for wound healing. However, it is the power density (brilliance) that is more important. This can be calculated using the formula:-
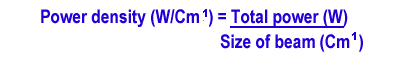
Using this, it can be calculated that the true laser has a greater power density (800 - 4000W/cm² ) than the SLD, where the power density is, on average, 50 - 75mW/cm² . Again, other facts need to be taken into consideration. For example, changing the pulse rate changes the number of fixed pulses in a specific time period. At 5Hz there are 5 pulses per second. At 5KHz there are 5000 pulses per second. As the rate increases, the radiant power output also increases, since each pulse contains a fixed number of photons. A pulsed SLD can therefore have as great a power as a simple true laser. Cluster units are also becoming common and for these it is essential to look at the sum of the individual effects. According to Baxter et al (1991), cluster units using SLD's have shown no obvious difference in effect from true lasers.
Another property that can be considered is coherence. With the true laser, the photons and waves are in phase, whilst SLD's produce incoherent light. However, it has been shown that the temporal coherence of a laser beam is mostly lost by the time the beam has passed through the first 1mm of tissue and that the property of coherence is of no significance at cellular level. Research by both Karu (1987) and Young et al (1989) has shown that coherence is not of importance when considering photo-biological reactions.
A more important aspect of comparing the two methods is that of laser-tissue interaction. High power and energy densities of the true laser can bring about strong thermal effects that are able to produce thermal coagulation and vapourisation. This lends them to surgical use. In contrast, the low power therapy is to a greater extent athermic. Although some thermal interactions do occur, the main interaction is photochemical, so that SLD's are an ideal clinical tool.
A major clinical application of the therapeutic laser is that of wound healing, since open wounds require lower energy densities. Considerable research has been carried out recently to find out why this irradiation stimulates the regenerative process. Firstly, the stages underlying the healing process were determined. Different aspects of the process were addressed by different groups. It has been shown that irradiation produces an increase in cell proliferation, essential for new growth to repair the wound.
Early work in this area was carried out by Hardy et al (1967) and has been continued at Guy's Hospital, London 1989. Collagen plays an important role in wound healing and it has been shown that irradiation by SLD's, (in this case GaAlA's), stimulates the production of collagen by fibroblasts (Lam et al 1986). In the same area, an increase in the proliferation of fibroblasts can be produced by the use of infra-red, as this stimulates protein metabolism (Toco et al 1985).
Synthesis of ATP (Adenosine Triphosphate) is also involved in the healing process. It has been shown that laser therapy can enhance ATP synthesis by stimulation of the respiratory/electron transport chain (Karn 1988). Furthermore, Inouie et al (1989), have shown that chronic wounds respond better after treatment with this therapy because it suppresses the immune reaction. As the immune response is involved in persistent chronic wounds, the healing process is accelerated.
This makes low energy laser therapy of use across a broad spectrum of applications. For the physiotherapist, it is an ideal treatment for ulcers. This includes trophic, varicose and diabetic ulcers as well as pressure sores (decubitus ulcers). Soft tissue injuries such as muscle tears and tendinopathies also have a good response, so that the treatment also is useful in sports medicine. In hospital use, post-operative wounds and burns also respond well to the treatment, at the same time giving a notable reduction in scarring. For the dental practice, laser therapy has been shown to reduce bleeding. It can also be of value in the treatment of cold sores and herpetic gingival stomatitis. In the case of alternative medicine laser acupuncture has been shown to be effective, as it is of benefit over metal needles when treating nervous patients or children. It also reduces the risk of the spread of HIV.
Veterinary practices also can gain from applying this form of laser therapy. In addition to soft tissue injuries and wound healing, it can be used to supplement treatment of respiratory tract infection if applied to the neck and underside of the throat. It has been used on horses to enhance the rate and texture of foot growth by irradiating the coronary band.
Although the application of low energy laser therapy has been shown to be a significant advantage when managing the treatment of wounds, research is now emerging to show the potential of this being applied to other areas. Infra-red diodes have been used to irradiate joints damaged by osteoarthritis and good results have been obtained (Trelles et al 1990). Pain relief has been effected in the treatment of tennis elbow using gallium arsenide emitters (Terashima et al 1990). There is also potential for low energy emitters to be used to alter the neurochemistry of both the central and the peripheral nervous system (Amemiya et al 1990).
While there are differences between true lasers and SLD's, it is clear that both produce physiological changes. SLD's are capable of doing the same job as many true lasers, with lowered risk of eye damage and at considerably lower cost. The important thing for the therapist to consider is the condition to be treated, the depth of penetration required and, taking power output etc. into account, to carefully calculate the optimum treatment duration.
June 1997 *Member of the Institute of Physics and Engineering in Medicine
